According to the Nci, What Are the Two Most Obvious Factors Related to Causing Health Disparities?
In 1928, Louis State of israel Dublin wrote "An comeback in Negro wellness, to the point where it would compare favorably with that of the white race, would at one stroke wipe out many disabilities from which the race suffers, meliorate its economic status and stimulate its native abilities as would no other unmarried comeback. These are the social implications of the facts of Negro Wellness" [1]. This compelling assertion remains valid to date. The fact that the African American population is the least healthy ethnic group in the USA is not due to chance. The first African Americans were brought to the Usa in chains equally slaves. The transport itself from Africa to the New Earth remains one of the best examples of the power of one sector of humanity to destroy the health of another. Estimates of the death charge per unit of slaves during the infamous "middle passage" are broad ranging, from approximately nine to 35 %. Slavery associated deaths were likely much college [ii, 3]
Once enslaved in what is at present the USA, African Americans were forced to live in physical and social conditions in which their health had very fiddling value. For more than than 250 years, enslaved African Americans suffered physical, social, and mental brutalization. The end of slavery did non hateful that African Americans could all of a sudden lead healthful lives. To the contrary, they take been subjected to systematic bigotry and oppression for the 150 years since slavery was abolished, and it continues nowadays. Healthwise, this history may be viewed as resulting in two outcomes. With so much suffering and early decease, those who survived this subjection may be the strongest and most resilient members of this group. All the same, the history of slavery and the current racial discrimination this group continues to suffer clearly underlie the inexcusably poor health condition of African Americans equally a whole.
In 1984, Margaret Heckler, and then Secretarial assistant of Health and Human Services (HHS), dissatisfied with the way health disparities were being reported to Congress, provided the first comprehensive review of wellness disparities endured by black and minority groups, compared with whites; the report laid the foundations for action to eliminate these disparities through health education, promotion, and access to health care. One of the most significant outcomes of the 1985 Report of the Secretary'southward Job Force on Black and Minority Health, also known as the Heckler Study, was the creation of the Office of Minority Health in 1986, with the mission "to improve the health or racial and ethnic minority populations through the development of wellness policies and programs that will eliminate health disparities." The Heckler Written report chosen health disparities among minority groups an affront both to our ideals and to the ongoing genius of American medicine [iv, 5].
Thirty years after the Heckler Written report was released, African Americans nonetheless endure unacceptable health disparities and lack the power over policy and deportment that could make the changes to eliminate such disparities. In this paper, nosotros review the scientific and "gray" literature on the health status of African Americans, using PubMed and government and not-regime sources. Our literature search was focused on by reviews and reports and is not a comprehensive review of contempo scientific enquiry on African American health, just a review of topics that the published literature identifies as existence the meridian priorities for improving the health status of blacks in the Us.
This review is guided by a modified social ecological model [half dozen, 7] that includes the social determinants of wellness, wellness disparities, main health needs, and admission to health services. Recommendations are offered to help frame policies and interventions to ameliorate African American health disparities. Our conceptual model allows us to chronicle social (distal) determinants, with individual (proximal) determinants of health (Fig. 1). Social determinants of health include the main variables of health inequalities, namely, race, poverty, and gender. These influence health needs (morbidity, mortality, and health risks). The social response to health needs is represented by health services (policies, access, utilization, and workforce), which in turn influences health needs and risks, by hopefully resolving or improving them. Given the amplitude of our model, we delimited content to top priorities, as supported past the relevant literature. A conceptual model or framework is not intended to represent a universal truth; its purpose and usefulness is to help cover and transform reality. Unidirectional, static relationships depicted in a framework practice not accurately reverberate the historical and social world we live in—including the health of African Americans—since social determinants of health are in turn influenced by the wellness status of the population; likewise, health risks influence the social determinants of health and modulate health policies and services. Health outcomes in turn alter wellness risks and influence the social response by wellness services. The relationship between social disparities on health status of disadvantaged population has long been documented, although a direct causal pathway remains elusive [8, 9]. In this complex causal network, social determinants of health include cultural mores that influence and are influenced by the wellness status of populations. It should be noted that the term "health disparities" is used in this paper indistinctly from "wellness inequalities"; the former being whatsoever imbalances in health burdening a particular subgroup of the populace [x] and the latter understood as unjust, unnecessary, and avoidable differences affecting mostly racial/ethnic, gender, and socioeconomic vulnerable groups [xi] While these terms can be semantically and conceptually distinguished, it is beyond the scope and infinite of this newspaper to do then. Also, the terms "blackness or African American" are used interchangeably to announce individuals that cocky-place as such, as used by the Us Census [12].
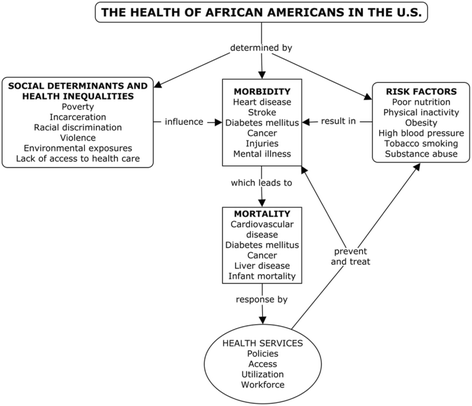
A conceptual map of the health of African Americans in the United states
The following sections present the principal components of African American health, every bit outlined in our conceptual framework: social determinants of health and health disparities, health needs (morbidity and mortality), health risks, and health services. Special emphasis is made on mental health and criminal and incarceration problems.
Social determinants of health and health disparities
In this department, we present the main social determinants of health disparities, namely, racism, poverty, pedagogy, housing, access to healthy foods, ecology exposures, violence, and criminal justice.
In 2014, African Americans numbered approximately 42.3 million, accounting for 13 % of the U.s.a. population. Near 55 % of them live in the Southern states. New York State has the highest number of blacks (3.eight meg), while the highest percentages are seen in the District of Columbia (50.6 %) and Mississippi (38.2 %) [xiii].
Racism is defined as "a belief that race is the main determinant of human traits and capacities and that racial difference produce an inherent superiority of a detail race" Footnote 1. It is well documented that race is a factor in health disparities that is not moderated by age, sex, and level of didactics [xiv]. Virtually, every cistron considered in this document is impacted by racism. For African Americans in the U.s., racism is a systemic, organized social and cultural miracle that, through exclusion, prejudice, and discrimination, is a cause of social and health disparities, manifested as both distal and proximal factors affecting wellness, for which measurements cannot always be defined [14].
Socially, racism is correlated with substandard employment, housing, education, income, and access to health services; associated risks include occupational hazards, exposures to toxic substances and allergens in the abode, depression-quality schooling, lack of availability of healthy foods, easy access to illicit drugs and booze, violent neighborhoods, and environmental exposures. Individually, racism exerts its deleterious effects through negative cognitive and emotional phenomena leading to psychopathology and morbidity, as posited past McEwen's Allostatic Load Model [xv, sixteen]. This model proposes that daily stressful life events diminish coping mechanisms also equally genetic makeup—through epigenetic effects—dissentious immune, hormonal, physiological, and neuronal systems from cradle to grave [17, 18].
Xxx per centum of African Americans believe that their health is dependent upon fate or destiny and only about 50 % experience that health is a high priority. Reception and utilization of health data are well-known major factors in disease prevention [19].
Fewer blacks graduate from high school (72.v %) than practice not-Hispanic whites (87.2 %) [twenty], and more whites than blacks earn a bachelor's degree (32.5 vs. 18.6 %). Every bit of February 2016, unemployment rates were twice as loftier for blacks (8.8 %) than for whites (4.iii %) [21, 22].
Poverty is a prime predictor for lacking basic human being essentials including acceptable clean water, nutrition, health intendance, instruction, clothing, and shelter [23]. African Americans are the poorest indigenous group in the U.s.. They have had the lowest median household income in the USA for the by 50 years: in 2014, measured at $35,398, compared to $53,657 for all races, and $74,297 for Asians [24]. Although African American income peaked in 2000, information technology has been declining e'er since. Poverty is highly correlated with poor health outcomes and increased morbidity and mortality. Middle disease, diabetes, obesity, elevated claret lead levels, and depression nascency weight are all more prevalent among poor individuals.
Many factors in the physical environs significantly influence the health of all populations including weather, topography, air quality, and vegetation. Many other homo-made influences also impact health and contribute to health disparities, just seldom receive adequate attention. The quality of housing affects health, and African Americans live in some of the country'south lowest quality housing. Asthma is related to poor housing, and African Americans are disproportionately affected from asthma. Segregated housing is correlated with a meaning increase in cardiovascular disease (CVD), and African Americans live in the nearly segregated conditions [25]. Location is likewise a wellness determinant, and African Americans live in the poorest neighborhoods with the highest rates of homicide. Persons who live in poor neighborhoods are too much less likely to gain the benefits of exercise considering of condom concerns.
Transportation is often a problem in poor communities, presenting obstacles to accessing wellness care services, especially preventive care, until emergencies arise.
Access to healthy foods is likewise a frequent problem in poor African American communities. "Nutrient deserts" depict neighborhoods without easy access to supermarkets that sell fresh produce and other healthy foods. Black neighborhoods take significantly fewer supermarkets than white ones. Several studies also document that the food that is available in poor black neighborhoods is less fresh and of lower quality. In contrast, booze outlets are much more numerous in black neighborhoods. Information technology is non surprising that rates of obesity and diabetes are highest in poor black neighborhoods [26].
Blackness people are significantly more likely to reside near sources of air pollution and a greater distance from air quality monitoring sites. African Americans are more than likely to live in a neighborhood in close proximity to a Superfund Footnote 2 toxic waste site. Such location has a wide negative health touch on. In these neighborhoods, hospitalization for diabetes is increased; there are many agin pregnancy outcomes—congenital centre defects, nervous arrangement defects, low nativity weight, renal dysplasia, etc. Childhood cancers are also increased in these settings. There is a xx–25 % increase in congenital anomalies among infants born in these communities [27].
Violence is as well a major determinant of health disparities. Information technology is a major crusade of injury, inability, and premature death. Black male person adolescents are six times more likely than whites to die of homicide, and firearms are the master method [28]. In 2009, blackness males accounted for sixty % of injuries due to firearms compared to viii % for whites [29]. At that place is a very significant lifelong inequity in exposure to violence for blacks vs. whites. Young blackness males are iv times more likely to die from a gunshot than their white peers.
In 2014, African Americans accounted for 13 % of the US population but over 57 % of the victims of homicide by firearm. Firearm homicide was the leading cause of decease for African American males ages xv–34, and the 3rd leading cause of death for Latino males in the aforementioned age group (and would be 2nd if combined with suicides in which firearms were used). Firearms were used in over 91 % of homicides of African American males ages 15–34 and in 81 % of homicides of Latino males in this age grouping [30]. It must also be noted that black children are twice equally likely to witness domestic violence and 20 times more probable to witness a murder than white children [31]. They are also more than likely to suffer maltreatment.
In that location are currently more than ii.iii one thousand thousand people housed in the nation'due south 1719 land prisons, 102 federal prisons, 2259 juvenile correctional facilities, 3283 local jails, and 79 Indian Country jails as well as in armed forces prisons, immigration detention facilities, civil commitment centers, and prisons in the US territories [32]. Approximately 50 % of all inmates in US jails and prisons are blackness, despite the fact that they represent less than xiii % of the population. Ane in six prisoners has a diagnosable mental illness. This population too suffers from infectious and chronic illness at rates that are four to 10 times higher than for the total population, including a rate of HIV infection that is 13 times that of the total population [33]. Non but exercise prisoners come from disproportionately poor populations, simply a lack of adequate healthcare has been well documented in many The states prisons and jails, despite the fact that this population has a constitutional correct to health services.
The number of women in prisons has been growing steadily from approximately 17,000 in 1980 (10 per 100,000 women) to 120,000 today (seventy per 100,000). Black females are imprisoned at a rate nearly three times as loftier as white females, and seven out of x imprisoned women have pocket-sized children.
The impact of incarceration on the family unit is devastating. 1 of every 15 blackness children has an incarcerated parent, compared to one of every 110 white children. Research has shown that children of incarcerated parents are six times more likely to be incarcerated themselves during their lifetimes [34]. More enquiry must be washed to improve our understanding of the long-term bear upon of this reality.
Because the boilerplate prison house term is less than 2.5 years, nigh 95 % of inmates will be released and will bring their wellness issues dorsum to their communities with them. Many of those released do not have health insurance, and in many states, are non eligible for Medicaid. In that location is a scarcity of rehabilitation programs for these individuals and inadequate attention to the resumption of basic rights such as voting. Information technology is not surprising, therefore, that 30–50 % of old prisoners become homeless after release. Despite the fact that correctional facilities provide an opportunity to attain groups often not reached by the health and social service systems, it is, instead, a major gamble factor for lifetime poor health [35].
Major health needs of African Americans
The measures commonly used to determine the health of populations and subgroups all tell the aforementioned story. In the United states, African Americans are the least good for you ethnic grouping. In looking dorsum at the progress made toward eliminating health disparities in Healthy People 2010, disparities between the not-Hispanic black population and the population with the all-time rates increased for 34 objectives (13 %). Ten of those objectives were for decease rates: neonatal and postneonatal deaths, boyish deaths, firearm-related deaths and homicides, diabetes-related deaths, and deaths due to HIV infection, coronary heart affliction, stroke, and cardiovascular disease among persons with chronic kidney disease.
A decrease in disparity was observed for 29 of the objectives (11 %); most of the decreases were institute in objectives addressing sexually transmitted infections and HIV. Below, we nowadays some of the main health indicators of wellness needs for African Americans [36].
Age-adjusted decease rates
Blacks had the highest age-adjusted death rate of whatsoever ethnic group in 2013 (1083.3 per 100,000 standard population for black males vs. 876.viii 100,000 for white males, the 2d highest). The rate for the total population was 731.9 per 100,000 population making the black male rate 48 % higher than the total.
Life expectancy and mortality
In the USA, from 1980 to 2014, life expectancy at nascence increased from 70.0 to 78.eight; 76.4 years for males and 81.two years for females. Life expectancy at birth for blacks is 75.2 years; 72 years for males and 78.ane years for females. The gap in life expectancy at birth between blacks and whites decreased from v.2 years in 2004 to 3.4 years in 2014. Betwixt 2004 and 2014, the mortality rate among 45–54-year-old black males decreased 28 % from 933.three to 671.viii deaths per 100,000 population, while the rate for white men did not change (511.two deaths per 100,000 population). Among 45–54-year-old black women, the mortality rate decreased by 18 % while it increased 11 % for white women [37, 38].
Years of Potential Life Lost (YPPL)
Overall, African Americans remain the to the lowest degree healthy ethnic population. At that place seems to have been marked comeback in this motion picture by 2010. African Americans ranked beginning in only 4 of the top 10 causes, but the listed causes had changed. Poisoning was added as a new cause and cirrhosis of the liver edged out HIV and diabetes (for both of which African Americans were number i) for the tenth spot.
Babe bloodshed rates
Perhaps black infant bloodshed provides the well-nigh transparent view of blackness health. Information technology has always been at least two.5 times greater than the white rate since information accept been recorded. The total rate for all ethnic groups has declined steadily since reporting was initiated, but the disparity between black and white infant mortality rates persists. Interestingly, there was a suspension in the decline for all ethnic groups from 2000 to 2005. This pause was due mostly to the increase in "preterm" and "very preterm" births past minority mothers. In 2005, the infant mortality rates were vi.86/100,000 for all births, five.76/100,000 for whites, and 13.vi/100,000 for blacks.
The decline recommenced for the catamenia 2005 to 2010. While the decline for the total population was 12 % during this flow, the black infant bloodshed declined sixteen %—the greatest pass up for whatever ethnicity [39]. However, the full US babe mortality rate was 5.96 infant deaths per thousand alive births in 2013, and that for African American infants was 11.1 per 100,000 alive births despite the recent progress [twoscore]. The low nascence weight (LBW) level was 6.98 % for non-Hispanic white women and xiii.08 % for non-Hispanic black infants in 2013. And, in 2013, the rate of preterm deliveries was 1.six times higher for African American women. In 2014, low nascency weight and preterm births before 37 weeks gestation were the highest amongst blackness women, 13.17 and xi.ane %, respectively [37, 41].
In 2002, blacks trailed whites in women receiving prenatal care in the get-go trimester (75 vs. 89 %) [42]. In 2008, only 59.1 % of African American women giving nascency to alive babies had any prenatal care vs. 72.2 % of white women. 11.v % of African Americans who received any prenatal care commenced in the third trimester [43].
Black women were also more than likely to report not receiving advice from their prenatal care providers most smoking abeyance and booze use. In that location was also less counseling regarding breast-feeding although the divergence was not significant in this study [44]. As noted above, the gap betwixt baby mortalities declined slightly between 2007 and 2010, only blackness infant mortality remains more than 200 % that of whites. Looking at the youngest mortalities, black infants have a significantly college neonatal and post-neonatal mortality than any other ethnic group [45].
Most sources indicate that more 75 % of all infants receive well babe intendance. Therefore, the differences in bloodshed are due to factors which have already made their bear upon at the time of birth, such equally the health status of the parents at conception, genetics, and environment [46].
Chronic diseases and homicide
Over contempo decades, 4 chief causes of morbidity stand up out: middle affliction, diabetes, cancer, and homicide. The black population displayed a larger subtract in death rates for heart disease, cancer, and HIV disease accounting for the narrowing gaps. Additionally, there was a larger subtract in unintentional injuries in black males.
Centre affliction is the leading cause of expiry for most Americans; 46 % of African Americans older than 19 years of age suffer from cardiovascular disease. According to the CDC, leading risk factors for center disease and stroke currently are loftier blood pressure, high cholesterol, diabetes, current smoking, physical inactivity, and obesity. Individuals with ii or more of these factors are at a higher risk for stroke and center illness. In 2003, the prevalence of two or more of these factors was highest in African Americans, and centre disease among African Americans has been the first or second cause of Years of Potential Life Lost in the USA e'er since these information have been kept. This disparity is not surprising given that African Americans had the highest prevalence of hypertension from 2007–2010; in 2011–2014, black men and women aged xx years and older continued having the highest prevalence of hypertension (42.4 and 44 %, respectively) [37]. African American women had the highest prevalence of obesity during this flow, and African Americans have had the highest rates of diabetes since the data have been collected. According to a 2014 report, blacks have a "ane.three-times greater rate of non-fatal stroke, a 1.eight-times greater rate of fatal stroke, a ane.5-times greater charge per unit of death attributable to eye affliction, and a 4.2-times greater charge per unit of stop-stage kidney disease" [47].
Cancer
When looking at all cancers, African Americans were the group nigh heavily impacted in 2012. Incidence rates were highest in the blackness population (554.five/100,000) and and so was the death rate (253.nine/100,000). Among women, however, the overall incidence rate for cancers is not the highest among ethnic groups, merely the death rate is.
A health disparity among women is best illustrated by breast cancer. While the incidence rate per 100,000 was lower for African American women (118) than for white women (133) and the total population (127), the death rate was highest amidst African American women at 33.eight per 100,000 vs. 25.5 for all women.
For African American males, the greatest cancer disparity is prostate cancer. For the menstruation 2000–2004, the incidence was 255.5 per 100, 000 vs. 161.4/100,000 for white males and 168/100,000 for the total population (Table ane) [48].
Homicides/interpersonal violence
When reviewing health disparities, homicides are always the cause of death with the largest ethnic disparity. It alternates with CVD as the greatest cause of YPLL for African Americans. From the menstruation 1999–2002, black males died from homicide at 10 times the rate of whites. In 2013, the age-adjusted homicide rate for blacks was 18.7 deaths per 100,000 population. This effigy was three times greater than the rate for whatever other ethnic group. While blackness males had the highest rate, black females had a college rate of homicide deaths than any other females, and intimate partner homicide was a major gene [49].
Homicide is the absolute measurement of violence, revealing the unquestionable ethnic disparity. However, violence affects African Americans in many other means. In 2013, college rates of aggravated assault, kid maltreatment, and fights among high school students were reported. In 2011, African American women reported higher rates of experiencing rape and concrete violence by an intimate partner [49].
Mental and behavioral wellness
National surveys show lower rates of mental disorders for blacks and Hispanics (xvi.9 %), as compared to whites (xix.3 %) [50]. However, more than blacks suffered serious psychological distress than whites in the previous year (6.9 vs. 4.4 %, respectively). That is to say, black people endure more than intense and frequent mental and behavioral health issues than their counterparts, at least in part related to poverty and exposure to racism and discrimination, both of which disproportionally affect minorities [51–53].
All the same, the proportion of youth who had serious thoughts of suicide was 40 % lower among black youth eighteen–25 years, compared to their white counterparts (5.0 vs. 8.2 %), and this highlights the resiliency needed for blacks for everyday survival.
Information technology has been shown that blacks receive fewer medication due to racial bias, low income, and insurance status. A study showed that blacks with depression and without insurance receive fewer antidepressants than those insured; even amongst the insured, they received fewer medication than whites [54]. Another study establish that fewer blacks receive opioids at discharge from emergency department visits due to back and abdominal pain, compared to whites [55]; also, information technology has been reported that substance abuse treatment centers serving higher percentages of minority populations prescribe fewer selective serotonin reuptake inhibitors (SSRIs) than centers serving fewer minority clients [56].
With respect to tobacco, African Americans have lower rates of employ than whites. For example, the 2013 NSDUH estimated that 27.6 % whites and 26.6 % blacks used tobacco products in the past calendar month [57]. However, analyses accept identified a crossover at age 29, whereby blacks terminate up with higher rates of tobacco use than whites, largely which were traced back to differences in educational attainment and marital condition [58]. Almost 30 years ago, the CDC concluded a report on racial disparities that reducing tobacco could pb to reducing wide wellness disparities in the following terms.
The reduction of cigarette smoking in the black population is one of the most of import, immediately bachelor options for reducing the wide disparities between the health status of minorities and that of whites [59].
Still, the inquiry discussed past the Surgeon Full general on the 50th Anniversary of the starting time Surgeon General Report on Tobacco showed that blacks keep to suffer a disproportionate brunt of tobacco-related mortality and morbidity [lx].
Obviously, much remains to be achieved when it comes to addressing the needs of the poorest communities in America, which are also those who suffer the highest rates of tobacco apply and tobacco-related consequences. Community-Based Participatory Research (CBPR) is a promising approach to aid overcome the lack of adequate smoking cessation programs for minority and underserved populations, such as the implementation of community-based smoking abeyance interventions that are peer-based and identify emphasis on behavioral alter grooming and social support, along with the use of nicotine replacement therapies and strategies toward stress management [61]. These and other efforts take advantage of federal and land-funded quit-lines that offering free counseling and nicotine replacement therapy to those interested in quitting tobacco. Yet, it is also necessary to acknowledge that the loftier cost of constructive medications has been an of import barrier to quitting tobacco among blacks and other minority groups.
The situation regarding drug use such as marijuana and cocaine is no dissimilar. Blacks have a slightly higher rate of past-calendar month use of marijuana as compared to whites (10.three vs. 8.7 %, respectively). Whites and blacks have like rates of past-month use of cocaine (0.half dozen %). However, the consequences of drug utilise disproportionally touch on blacks. For example, blacks take higher rates of DSM-Four substance corruption/dependence to illicit drugs than whites (4.i vs. 2.4 %, respectively, in the past yr), merely not of booze abuse/dependence (six.0 vs. 6.5 %, respectively). Only one third to one fourth of people in need of addictions treatment got it, at least as reflected in the latest national survey of drug use. The bear on of substance use and mental wellness bug is evident in other social domains. For example, in 2014, there were 619,809 arrests due to marijuana possession (39.7 % of all drug arrests) (http://www.drugwarfacts.org/cms/Marijuana#Full). Blacks were almost four times more likely than whites to exist arrested for marijuana, in spite of the fact that both groups have relatively similar apply rates equally shown earlier [62].
Near two out of three people with whatsoever mental disease also had alcohol or drug dependence (66.eight %). Yet, among blacks, only two out of three people with Major Depressive Episode (MDE) received any form of treatment (64.6 %), and 1 in four people with severe MDE and damage did not receive treatment (26.iii %). Overall, 55.three % of Americans with an unmet mental health need did not receive treatment or counseling in the past year, reporting that they "could not beget the cost," 25.v % "did not know where to go," and 24.six % thought they "could handle the problem without treatment" [50]. While we cannot break down these data to clarify possible racial and indigenous differences, it is important to also consider that stigma has been major factor in blacks not receiving mental wellness care and may further complicate the effect of other healthcare barriers [63–66].
In sum, the data draw a rather complex moving picture in which blacks mostly accept similar if not lower incidence rates of mental disorders and substance interest than whites, simply at the same time suffer college prevalence of serious mental health and legal problems, with devastating furnishings. The difference betwixt lower incidence and college prevalence derives from longer elapsing, given lower access and utilization of healthcare services, lower quality of healthcare services, and worse complications of comorbidities for minority and underserved populations, amid others [56, 67–72]. In convergence, the greater impact of mental health issues for blacks stems from structural factors that include poverty, racism and discrimination, and civilization [73–75], such that the stress caused past the interaction of poverty, inequality, and discrimination affects blacks above and across of the effect on other non-minority populations. Clearly, several barriers demand to be lifted if nosotros are to make progress in this area, start by providing expanded true admission to healthcare services including transportation, availability of culturally friendly services, and the establishment of mechanisms that will avoid stigmatizing clients and ensure confidentiality of the data [51].
Unfortunately, a growing trunk of research documents that dr. bias leads to a lower quality of care for CHD based on patient'south race/ethnicity, sometimes patient gender, and his/her socioeconomic status [76].
Health care services: policies, access, and utilization
In this section, we review the social response to health needs of blacks, equally implemented through policies and programs, as well as issues of access and utilization. The role of an educated and culturally sensitive workforce is highlighted.
In 2003, the Institute of Medicine released Unequal Treatment: Against Racial and Indigenous Disparities in Health Intendance, a comprehensive review of disparities in healthcare treatment. The attitude expectations and behaviors of providers and patients were examined. Conscious and unconscious differences in handling based on ethnicity, socioeconomic status, and gender were reviewed. This document reviewed the biases, stereotypes, and advice obstacles impacting the interaction of providers and patients and their utilization of the healthcare organisation. Findings in the report concluded that:
"Bias, stereotyping, prejudice, and clinical uncertainty on the office of healthcare providers may contribute to racial and ethnic disparities in healthcare"; and that, "a modest number of studies suggest that racial and ethnic minority patients are more likely than white patients to reject treatment" [77].
In recent years, blacks have had worse access to care than whites for almost one-half of access measures used. During the first one-half of 2014, the percent of adults ages 18–64 without health insurance decreased more quickly among blacks and Hispanics than whites, only differences in insurance rates betwixt groups remained.
In March of 2010, President Obama signed in to police force the Patient Protection and Affordable Care Act (ACA) to increment the quality and affordability of wellness care by increasing access to insurance. This plan aims to increment healthcare protection by expanding coverage, property insurance companies answerable, decreasing healthcare costs, allowing provider choice, and enhancing the quality of care [78].
Nearly eight million African Americans obtained access to expanded preventive services, and nearly eight million African Americans with a preexisting health condition became able to obtain coverage. Since the first quarter of 2015, the uninsured rate dropped by 9.two per centum points among African Americans in the 18–64-year-sometime age group. Approximately 5.7 million young adults gained coverage from 2010 through March 4, 2015, dropping the immature adult uninsured rate by 7.4 % [79, fourscore].
The ACA is irresolute the funding of hospitals from a arrangement based on quantity of patients and procedures to one focused on quality of care—value instead of volume. Now, many of the responsibilities that have traditionally been those of public health are incorporated into the "Community Health Plan" of the hospital and expansion of Medicaid. This change in the basic protocol of healthcare delivery in the Us offers a significant opportunity for African Americans and other under-represented and minority groups to insert themselves into the wellness care infrastructure [81].
Withal, not all states accept undergone Medicaid expansion under the ACA, with negative consequences for admission and the wellness status of minorities and the poor. Texas and Mississippi—states with college percentages of black populations—are among the 17 that have rejected Medicaid expansion [82]. According to the Kaiser Foundation, 40 % of eligible blackness adults live in states rejecting Medicaid expansion and are ii-fold more likely than whites and Hispanics to remain uninsured [83].
Also, a report showed that, in states not expanding Medicare, low income adults aged 18–64 were more likely to be black and reside in rural areas than in states expanding Medicare; also, they were less likely to have a usual source of care and apply preventive services (dental checkups, routing checks, flu vaccinations, and blood pressure checks) [84].
Health workforce
An educated and informed black population will use health care services more effectively. Forty percent of African Americans have limited reading skills [85]. Health literacy is 1's ability to obtain, procedure, and understand basic wellness information and services. This skill is necessary to make appropriate health decisions. Good wellness literacy requires the reading, analysis, and controlling skills to make advisable health decisions. Lack of wellness literacy skills is considered a cause of health disparities, and disparities by both race and educational condition when health literacy are taken into account [86]. People with poor health literacy take problems communicating with their health providers, reading instructions on medicines, and completing medical and insurance forms.
In 2012, blacks were 13.6 % of the "working age population" but were not xiii % of any of the major health professions. In the present, only 5.3 % of active physicians are black, and that is truthful for 10 % of nurses. Oral health remains a major issue for African Americans, just only three % of dentists are black.
As we look more broadly at clinical providers, we encounter that only v.two % of advanced exercise registered nurse (APRN), viii % of dr. assistants (PA), and ~5 % of pharmacists are blackness. Expanding the view fifty-fifty further, only 4 % of occupational therapists and spoken language therapists are African American.
Historically Black Colleges and Universities (HBCUs) have been a major educational resource for African Americans since the end of slavery almost 150 years ago. The primary mission of HBCUs is to educate blackness Americans. There are currently 100 HBCUs, and about xxx % of the BA degrees awarded to African Americans annually are produced past the 89 4-year HBCUs.
In 2010–2011, blacks earned 85 % of the 33,000 available's degrees conferred by HBCUs and 73% of the master'due south degrees. From another perspective, HBCUs awarded 35 % of the bachelor's degrees to blacks in the USA in 1976–1977. This figure dropped to 16 % in 2010–2011. Facing the increasing need for health professionals, there has been a meaning expansion of health training programs across the The states. Information technology is stunning to see that wellness programs in HBCUs have not shared in this growth. In 2007, only v % of full-fourth dimension faculty members at higher instruction institutions were black [87]. In 2011, not-blackness students made up nineteen % of enrollment at HBCUs. In 2013, only lx % of nurses trained in HBCUs were African American [88].
The future
This section presents the key messages the authors would like to convey regarding social determinants of health and wellness disparities, health needs, and healthcare policy and services, to ameliorate the health of African Americans in the Us
Given all that has been detailed, it is obvious that there is much to be done if nosotros are ever to achieve health equity or eliminate health disparities in the USA and assure good health to the African American population. A goal of Salubrious People 2010 was the "elimination" of health disparities. Information technology was not accomplished for African American people [89]. The current picture is clear; the greatest health disparity betwixt the total Us population and any ethnic group is establish in African Americans.
Every bit stated in the introduction, racism may be the most important phenomenon underlying black health disparities, exerting its ominous effects through institutionalized, systematic stigma and exclusion. Equally we have shown, health disparities for blacks are racial disparities; social and gender disparities are interwoven and magnified to render blacks the least good for you of all groups. Historically structured racist practices and institutions are further reproduced by white-majority policymakers, conclusion makers, administrators, educators, and healthcare providers. Addressing "health disparities," "cultural competence," and "racial bias" at the individual level through healthcare services misses the social, institutional, and organizational levels underlying health disparities among blacks. At the individual level, this focus is translated into insufficient allocation of resources to black communities and populations [xc].
Poverty, low education, unemployment, violence, insecurity, and ecology exposures contribute to poor reproductive wellness and nascence outcomes amidst black women [90]. These factors impact the woman and her family at multiple levels: low access to salubrious foods, inadequate access to preventive and antenatal healthcare, intimate partner violence [91], distrust of the justice and police organization [92], unhealthy behaviors, substance corruption [93], and stress [94].
A greater proportion of black children are born and live in this social, environmental, and culturally deprived environment; thus, they grow and develop unequally—socially, psychologically, and healthwise, throughout the lifespan [95].
Research into minority and black health issues has been found to be both insufficient and biased [96].
The systemic nature of racism as a cause of wellness disparities must be counteracted by equally systemic measures, through social programs, economical investment, criminal system reform, decreased segregation in positions of institutional power, more inclusive research and appropriate funding of public agencies, healthcare institutions, and HBCUs [90, 97]. Further implementation and expansion of the Affordable Care Act should event in improved health outcomes for black populations [98].
Of course, addressing the wide ranging consequences of poverty is a social problem that all those working for health equity must endeavor to redress. Although in that location has been significant progress in assuring healthcare for the poor with the ACA and other programs, health institutions must non pretend that adequate healthcare is available to all. The care that is provided to all must exist of the highest quality, non only technically merely ethically. Physicians and public health professionals, black and otherwise, must correspond racial and social justice [99]. Proactive efforts must be taken throughout health systems to eliminate the conscious and unconscious differences in the quality of care currently provided in all aspects of medical practice. These efforts must exist directed at the do of all health providers and the performance of all systems [100].
Public health should take the lead in advocating for and providing the expertise to assure that inadequacies in physical and social environments do not harm African American populations. In the physical environs, priorities include informing at-risk populations of the impacts of their unhealthy environments, balls of good housing and transportation, and documenting the location and bear on of toxic waste product; these interventions should be approached through cross-sector collaborations [101].
The health of persons under the control of judicial and incarceration systems may be ane of the highest priorities in the social arena. A concentrated endeavor to educate and train justice organization administrators and staff in the basic principles of health care is necessary, and the provision of wellness services should be overseen by an unbiased body which is independent of the justice arrangement. Information technology has been demonstrated that healthcare systems based outside prison walls can provide first-class healthcare to inmates and eliminate the barriers which prevent returning convicts from receiving advisable care upon release [102].
Many strategies such every bit advocating for the appropriate location of supermarkets and farmers' markets and promoting of inner city community gardens tin can take a significantly positive impact on the health of African Americans [103].
Addressing the problems of diet and food deserts should be loftier priorities. Diabetes, CVD, and obesity will be directly affected, while many other major health problems in the African American customs will exist impacted [104, 105].
Many other disparities contribute to the poor health status of African Americans. Depending on how "crusade of death" is determined and how it is calculated, diabetes is often in the top x causes of morbidity and mortality for African Americans. The aforementioned tin can be said for substance abuse, lung cancer, and stroke. African Americans are over-represented when the top x causes of Years of Potential Life Lost are documented. Mental illness is a major problem, but much work needs to be done to develop an accurate and useful picture of the overall disparity [106].
Access to preventive, curative, and rehabilitative care must be bodacious to all persons including African Americans. Access is a lifelong demand. Treat the potentially pregnant women is crucial and may have long-term consequences for her and her offspring. Comprehensive care for the babe, kid, and boyish is the primal to their lifelong health and also their ability to function as productive and creative people. Adults oftentimes must be reminded that there are standards for healthcare from which they will benefit, and, as the population ages, access to advisable and comprehensive care must be assured for elderly African Americans.
In gild to assure intendance of the highest quality, proactive efforts must exist taken throughout health systems to eliminate the conscious and unconscious differences in quality of intendance provided. These efforts must be directed at the practice of all health providers and all systems. Today, the differences are integral to virtually all health practice [107].
Education at all levels may exist the well-nigh of import role of health professionals. Information technology is our responsibility to translate our knowledge of health into the language and culture of the client we are serving. Minorities are more likely to seek intendance from healthcare professionals of their own ethnicity. Communities are more willing to collaborate with providers in taking on this chore [108].
The development of health policy is most often the responsibility of those with no health expertise, with little representation of the black population. Without the education of health professionals who are knowledgeable of the culture of African American communities and committed to their well-beingness, the future of policy development is dour [109]. HBCUs have played a major role in a variety of fields in the 150 years of their existence and are not being appropriately utilized in the training of black health professionals.
Likewise, the policies of health exercise and health institutions that serve African Americans are nearly oft adamant by public and individual sector leaders who accept no wellness training. It is the responsibleness of trained health professionals to provide the data needed to make appropriate health policy decisions and to evaluate their implementation. In addition to these factors, communities, providers, and individuals must all empathise that politics is a key factor in the ongoing battle to eliminate the disparities in wellness outcomes in the Usa that are based on racial differences.
Source: https://publichealthreviews.biomedcentral.com/articles/10.1186/s40985-016-0025-4
0 Response to "According to the Nci, What Are the Two Most Obvious Factors Related to Causing Health Disparities?"
Post a Comment